Cholesterol Management
Optimal cholesterol management is an important part of reducing atherosclerotic cardiovascular disease (ASCVD). Evidence-based treatments are readily available. Treatment protocols and decision aids can assist clinical teams and their patients in making informed decisions that can lead to fewer heart attacks and strokes.
Featured Resource
For people with high LDL cholesterol levels or for others at high risk for having an ASCVD event in the next 10 years, experts recommend lifestyle changes and cholesterol-lowering medications to lower ASCVD risk. Clinical blood cholesterol treatment guidelines released in 2013 from the American College of Cardiology (ACC) and the American Heart Association (AHA) recommended statins for four main groups who might benefit.1
In November 2018, new clinical guidelines were released by the ACC, AHA, and others that provide additional specificity to the 2013 recommendations, reinforce the need for appropriate-intensity statin therapy among people at risk of having an ASCVD event, and emphasize the importance of patient–clinician shared decision making.2
About Cholesterol
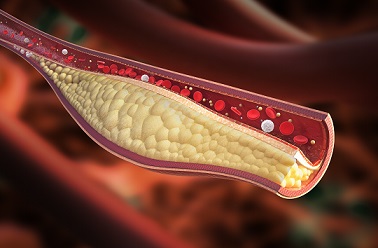
Cholesterol is a waxy, fatlike substance. It is produced by the liver and is present in dietary sources. It is a major component of cell membranes and is used to make hormones, vitamin D, and bile acids used in digestion.
Cholesterol is carried through the blood on lipoproteins. There are two major types of lipoproteins:
- High-density lipoprotein (HDL), often called “good” cholesterol
- Low-density lipoprotein (LDL), often called “bad” cholesterol
Excess LDL cholesterol is deposited in the walls of arteries throughout the body. This can lead to ASCVD, which includes heart attack, stroke, transient ischemic attack (TIA), stable or unstable angina, and peripheral artery disease (PAD), including aortic aneurysm, all of atherosclerotic origin.
As many as 1 in 212 U.S. adults may have a genetic condition called familial hypercholesterolemia (FH), an inherited disorder that causes the liver to have problems metabolizing and removing excess LDL cholesterol, resulting in very high LDL levels.3 This can lead to premature ASCVD. Recommended treatment for FH includes healthy lifestyle choices and statin therapy, started early and continued with close follow-up to reach treatment goals. Experts estimate that at least 90% of people with FH have not been properly diagnosed4 and that FH accounts for approximately 5% of all annual myocardial infarctions in Americans under age 60.5
About Statins
Statins, or HMG-CoA reductase inhibitors, lower LDL cholesterol by reducing the liver’s production of cholesterol. They also improve the liver’s ability to remove LDL cholesterol that is already in the blood.6
Data from 2013–2014 indicate that only about half (54.5%) of U.S. adults (over age 21) who might benefit from statin use are taking them. Some groups are more likely to use statins for cholesterol management than others:
- Eligible adults over age 65 are more likely (63.5%) than adults ages 35–64 (48.1%) to use statins.
- Non-Hispanic white adults are more likely (58.3%) than non-Hispanic black (44.3%) or Hispanic (33.7%) adults to use statins.7
The 39.1 million people who are at high risk for an ASCVD event but are not taking a statin could reduce their risk of a heart attack or stroke by up to half if therapy were taken regularly.7,8 Clinicians and patients should weigh this significant potential benefit against the small risk of experiencing harmful side effects:

- In rare instances, statins may cause myopathy, which is muscle damage often associated with the release of enzymes into the blood. Approximately 10% to 25% of patients treated in clinical practice report muscle symptoms (aches, weakness) after initiating statins, but multiple large-scale blinded randomized controlled clinical trials found no differences in the frequency of muscle symptoms between participants on a statin and those on a placebo.9The discrepancy between observational clinical experience and randomized trials is likely due to patients’ and clinicians’ inappropriately attributing muscle problems to statins in clinical practice, possibly due to the “nocebo” effect, where patients experience side effects because they anticipated doing so.9,10 There are practical approaches to managing reported muscle symptoms.11
The 2018 ACC/AHA guidelines state that very high-risk individuals who have suboptimal LDL levels after maximal doses of statins may also benefit from additional medications:
- Ezetimibe. This medicine reduces blood cholesterol by limiting the absorption of cholesterol by the small intestine. This reduces how much cholesterol travels from the intestine to the liver, lowering the amount of cholesterol that is stored in the liver and increasing the amount of cholesterol cleared from the blood.12
- PCSK9 inhibitors. The PCSK9 protein helps determine how much cholesterol is absorbed by the liver. Overactive PCSK9 proteins prevent the liver from absorbing as much cholesterol as it could.13 PCSK9 inhibitor medications, which are administered by injection, attach to PCSK9 proteins, disabling the overactive proteins and allowing the liver to absorb more cholesterol from the blood.14
- Bile acid sequestrants. These medicines help remove cholesterol from the blood by removing bile acids. The body needs bile acids, and removing them forces the liver to make more, which it does by breaking down LDL cholesterol, consequently lowering serum cholesterol levels.6
Tools and Resources
For Clinicians
- Cholesterol Management Change Package (CMCP) [PDF – 1 MB]
The CMCP was developed in partnership with the National Association of Community Health Centers (NACHC) and the American Medical Association (AMA). It presents a list of evidence-based process improvements that outpatient clinical settings can implement as they seek optimal cholesterol management. - 2018 ACC/AHA/AACVPR/AAPA/ABC/ACPM/ADA/AGS/APhA/ASPC/NLA/PCNA Guideline on the Management of Blood Cholesterol
These updated guidelines provide additional specificity to the 2013 recommendations, reinforce the need for appropriate-intensity statin therapy among people at risk of having an ASCVD event and emphasize the importance of patient–clinician shared decision making. - ASCVD Risk Estimator
This risk estimator calculates the estimated 10-year and lifetime ASCVD risk among patients without ASCVD. - Statins Infographic in English [PDF – 214 KB] and Spanish [PDF – 244 KB]
This infographic explains the role that statins play in reducing LDL cholesterol. - FH Foundation Familial Hypercholesterolemia Diagnosis, Management, and Family Screening
This clinical resource provides information about the diagnosis and management of familial hypercholesterolemia. - CDC Cholesterol Communications Kit
These social media messages and graphics can help your patients understand what cholesterol is and why managing cholesterol is important for reducing the risk of cardiovascular disease.
For Patients
- Statins Infographic in English [PDF – 214 KB] and Spanish [PDF – 244 KB]
This infographic explains the role that statins play in reducing LDL cholesterol. - The Scoop on Statins: What Do You Need to Know?
This Q&A helps people with high cholesterol understand not only the importance of taking a statin for heart attack and stroke prevention but also the facts about side effects. - Cholesterol
CDC’s cholesterol website contains plain language information for patients, including what cholesterol numbers mean and healthy lifestyle changes that can help lower cholesterol. - Mayo Clinic Statin Choice Decision Aid
This resource helps patients and their doctors discuss how they might want to reduce risk for heart attacks. - Cholesterol and Statins
This infographic from the Food and Drug Administration helps explain cholesterol basics. - Familial Hypercholesterolemia
This fact sheet from the FH Foundation helps explain more about this condition. - The short animated video below can help people understand how statins prevent heart attacks and strokes by lowering their cholesterol levels.
References
- Stone NJ, Robinson JG, Lichtenstein AH, Bairey Merz CN, Blum CB, Eckel RH, et al. 2013 ACC/AHA guideline on the treatment of blood cholesterol to reduce atherosclerotic cardiovascular risk in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol. 2014;63(25 Pt B):2889–934.
- Grundy SM, Stone NJ, Bailey AL, Beam C, Birtcher KK, Blumenthal RS, et al. 2018 ACC/AHA/AACVPR/AAPA/ ABC/ACPM/ADA/AGS/APhA/ASPC/NLA/PCNA guideline on the management of blood cholesterol: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Clinical Practice Guidelines. J Am Coll Cardiol. 2018.
- Bucholz EM, Rodday AM, Kolor K, Khoury MJ, de Ferranti SD. Prevalence and predictors of cholesterol screening, awareness, and statin treatment among US adults with familial hypercholesterolemia or other forms of severe dyslipidemia (1999–2014). Circulation. 2018;137(21):2218–30.
- Nordestgaard BG, Chapman MJ, Humphries SE, Ginsberg HN, Masana L, Descamps OS, et al. Familial hypercholesterolaemia is underdiagnosed and undertreated in the general population: guidance for clinicians to prevent coronary heart disease: consensus statement of the European Atherosclerosis Society. Eur Heart J. 2013;34(45):3478–90a.
- Knowles JW, O’Brien EC, Greendale K, Wilemon K, Genest J, Sperling LS, et al. Reducing the burden of disease and death from familial hypercholesterolemia: A call to action. Am Heart J. 2014;168(6):807–11.
- Cholesterol-lowering medicine. https://www.cdc.gov/cholesterol/treatment/index.html. Updated October 31, 2017. Accessed October 18, 2018.
- Wall HK, Ritchey MD, Gillespie C, Omura JD, Jamal A, George MG. Vital Signs: Prevalence of key cardiovascular disease risk factors for Million Hearts® 2022 — United States, 2011–2016. MMWR. 2018;67(35):983–91.
- Cholesterol Treatment Trialists’ (CTT) Collaboration. Efficacy and safety of more intensive lowering of LDL cholesterol: a meta-analysis of data from 170 000 participants in 26 randomised trials. 2010; 376(9753):1670–81.
- Ganga HV, Slim HB, Thompson PD. A systematic review of statin-induced muscle problems in clinical trials. Am Heart J. 2014;168(1):6–15.
- Tobert JA, Newman CB. The nocebo effect in the context of statin intolerance. J Clin Lipidol.2016;10(4):739–47.
- Rosenson RS, Baker S, Banach M, Borow KM, Braun LT, Bruckert E, et al. Optimizing cholesterol treatment in patients with muscle complaints. J Am Coll Cardiol. 2017;70(10):1290–301.
- Food and Drug Administration. ZETIA® (ezetimibe) tablets drug label. https://www.accessdata.fda.gov/drugsatfda_docs/label/2008/021445s019lbl.pdf [PDF – 202K]. Updated September 2007. Accessed October 18, 2018.
- National Library of Medicine. PCSK9 gene. Genetics Home Reference. Rockville, MD: National Institutes of Health; 2018. https://ghr.nlm.nih.gov/gene/PCSK9#conditions. Updated October 16, 2018. Accessed October 18, 2018.
- Jin J. PCSK9 inhibitors for treating high cholesterol. JAMA. 2015;314(21):2320.
