Cardiac Rehabilitation Change Package (Second Edition)
What Is the Cardiac Rehabilitation Change Package (CRCP)?
The CRCP was developed in partnership with the American Association of Cardiovascular and Pulmonary Rehabilitation (AACVPR) to present a listing of process improvements that CR champions can implement as they seek optimal CR utilization. It is composed of change concepts, change ideas, and tools and resources.
- Change concepts, sometimes called key drivers, are general notions that are useful in the development of more specific ideas for changes that lead to improvement.
- Change ideas are actionable, specific ideas or strategies for changing a process. Change ideas can be rapidly tested on a small scale to determine whether they result in improvements in the local environment.
- With each change idea, the CRCP lists one or more evidence- or practice-based tools and resources that can be adapted by or adopted in a health care setting to improve CR utilization.
The purpose of the CRCP is to help quality improvement teams from hospitals and CR programs implement systems and strategies that target improved care for more patients eligible for CR.
The CRCP was originally published in 2018 and was used by hospital and CR program staff to increase CR participation for five years. The second edition, published in 2023, includes new change concepts, change ideas, and twice as many tools and resources that reflect the latest evidence and experience of hospitals, CR programs, and national organizations and quality improvement organizations. Specifically, the second edition of the CRCP includes new content to:
- Communicate the opportunity for improvement to hospital leadership
- Access and use data to drive improvement
- Develop new CR program staffing models
- Implement automatic “opt out” referrals with care coordination (largely generated from the Agency for Healthcare Research and Quality’s TAKEheart initiative),
- Increase CR participation among people from demographic groups historically underrepresented among CR participants
- Advance hybrid CR delivery models
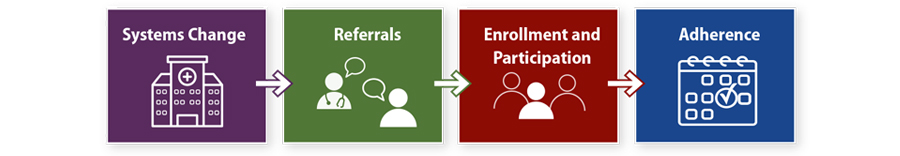
The second edition uses the notation (New) to identify new tools or resources added to those from the first edition, (SET) to demark tools or resources that may be adapted to increase participation in supervised exercise therapy (a separate and distinct service that can be delivered at CR program facilities and can benefit individuals with specific cardiovascular disease diagnoses), and (HE) to highlight tools or resources that address the characteristics of equitable quality care. The CRCP is broken down into four main focus areas:
How Should We Use the CRCP?
Start by bringing together a team of CR professionals, physicians, administrators, and other relevant stakeholders to discuss the aspects of CR utilization that are most in need of improvement. The team can then select corresponding interventions from the CRCP that best address those issues.
Each strategy you choose should first be tested on a small scale (i.e., conduct “small tests of change”) to assess feasibility and allow the team to evaluate and adjust before instituting the change on a broader, more permanent scale.
We do not recommend implementing all of the interventions at once, nor is it likely that all interventions will be applicable to your clinical setting.
Million Hearts® partnered with the National Association of Chronic Disease Directors to develop a 4-part video series to provide insights and tips from cardiac rehabilitation champions to implement high impact strategies and/or adapt or adopt featured tools from the CRCP.
Spread the Word
Use the following content to promote the CRCP through your personal or professional channels.
Facebook/LinkedIn
- Ready to improve #CardiacRehabilitation participation in your hospital or health system? Download the Million Hearts [tag] and AACVPR [tag] change package for ideas and resources to get started. https://bit.ly/2EdKeNp #CRSavesLives #MillionHeartsQI
- Despite its lifesaving benefits, many eligible patients do not enroll or participate in #CardiacRehabilitation. Improve enrollment and participation rates with evidence-based tools from the Million Hearts [tag]/AACVPR [tag] Cardiac Rehabilitation Change Package. https://bit.ly/2EdKeNp #CRSavesLives #MillionHeartsQI
- Evidence shows that #CardiacRehabilitation benefits patients after a cardiac event or procedure. Implement interventions from the Million Hearts [tag]/AACVPR [tag] Cardiac Rehabilitation Change Package. https://bit.ly/2EdKeNp #CRSavesLives #MillionHeartsQI
- Ready to improve #CardiacRehabilitation participation in your hospital or health system? Download this @MillionHeartsUS/@AACVPR change package for ideas and resources to get started. https://bit.ly/2EdKeNp #CRSavesLives
- Despite its lifesaving benefits, many eligible patients do not participate in #CardiacRehab. Improve participation rates with evidence-based tools from this change package. https://bit.ly/2EdKeNp #CRSavesLives #MillionHeartsQI
- Evidence shows that #CardiacRehabilitation benefits patients after a cardiac event or procedure. Implement interventions from the @MillionHeartsUS/@AACVPR Cardiac Rehabilitation Change Package. https://bit.ly/2EdKeNp #CRSavesLives
Newsletter Content
Include this language in your communications:
CDC’s Division for Heart Disease and Stroke Prevention is pleased to announce the release of the second edition of the Million Hearts®/American Association of Cardiovascular and Pulmonary Rehabilitation Cardiac Rehabilitation Change Package, available at: https://millionhearts.hhs.gov/files/Cardiac_Rehab_Change_Pkg.pdf [PDF – 880 KB]
We invite you to share this resource with cardiac rehabilitation (CR) program staff, hospital quality improvement teams, and public health professionals who partner with these groups to implement strategies that improve care for CR-eligible patients.
Shareable Graphic

Learn More
Acknowledgements and Contributors
Million Hearts® and AACVPR would also like to acknowledge the contributions of the Agency for Healthcare Research and Quality’s TAKEheart initiative, specifically Dina Moss, MPA, and Michael Harrison, PhD, of the Agency for Healthcare Research and Quality, the team at Abt Associates, the 18 technical expert panelists, the 14 members of the Hybrid Cardiac Rehabilitation Work Group, the 60 TAKEheart Training Curriculum and Learning Community contributors, the 120+ TAKEheart Partner Hospitals, and 850+ members of the TAKEheart Learning Community.
For More Information
Haley Stolp, MPH
Division for Heart Disease and Stroke Prevention,
Centers for Disease Control and Prevention
hstolp@cdc.gov
Suggestion Citation
Centers for Disease Control and Prevention. Cardiac Rehabilitation Change Package, Second Edition. Atlanta, GA: Centers for Disease Control and Prevention, US Department of Health and Human Services; 2023.

